The Lung Center Provides Specialized Treatment for TBM
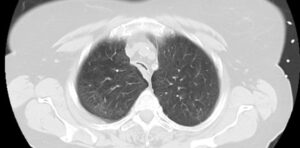
An often-misdiagnosed lung condition is receiving special attention from a multidisciplinary team of specialists at The Lung Center at Brigham and Women’s Hospital.
Latest Clinical & Research News
Specialty: Pulmonary & Thoracic Surgery

An often-misdiagnosed lung condition is receiving special attention from a multidisciplinary team of specialists at The Lung Center at Brigham and Women’s Hospital.
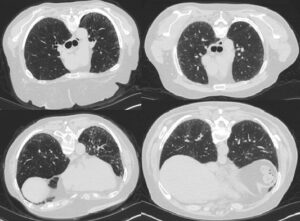
Idiopathic pulmonary fibrosis (IPF) is more common than once thought. According to the American Lung Association, over 130,000 people are affected in the United States and about 50,000 new cases are diagnosed each year.

Asthma and chronic obstructive pulmonary disease (COPD) each affect millions of people in the United States. So it’s not unexpected that a subset of patients would have both lung conditions. Yet surprisingly, little is known about the science of what’s called asthma-COPD overlap, or ACO. Experts at Brigham and Women’s Hospital are focused on changing that.
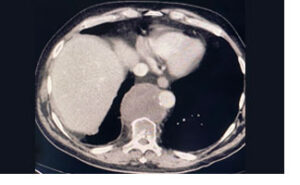
In the summer of 2019, Paul Pezzote, 67, learned he had Stage 4 cancer. Pezzote, who has Parkinson’s disease, had undergone treatments in 2010 at Dana-Farber/Brigham and Women’s Cancer Center (DF/BWCC). However, the cancer had returned and spread.

In March of 2020, Brigham and Women’s Hospital purchased four additional extracorporeal membrane oxygenation (ECMO) machines to prepare for a possible surge of COVID-19. It wasn’t yet clear if ECMO could support critically ill COVID-19 patients, but early reports from China had shown promise.
SARS-CoV-2 and influenza A (H1N1) are in the same category of virus and both infect the respiratory tract. However, research has shown distinctive vascular changes in the lungs of patients with COVID-19 compared to those with H1N1.
Prone ventilation is well-established as an essential treatment for mechanically ventilated patients with moderate to severe acute respiratory distress syndrome (ARDS). Since the start of the COVID-19 pandemic, clinicians at Brigham and Women’s Hospital have been investigating the impact of proning awake individuals with ARDS before intubation.
Anthony Francis Massaro, MD, director of the Brigham’s Medical Intensive Care Unit, said that early initiation of prone ventilation in mechanically ventilated ARDS patients enhances oxygenation via several mechanisms. Read More
A decision by Brigham and Women’s Hospital in the early days of the COVID-19 pandemic is helping patients hospitalized with the virus avoid two potentially fatal complications: deep vein thrombosis (DVT) and pulmonary embolism (PE). The Brigham’s protocol to give all hospitalized patients a prophylactic anticoagulant dose of low-molecular-weight heparin (LMWH) addresses blood clot risk factors that are particularly acute in patients with COVID-19. Read More
 Dr. Matthew Rochefort and Dr. Anthony Coppolino prepared to perform a bedside percutaneous tracheostomy in a COVID+ patient.
Dr. Matthew Rochefort and Dr. Anthony Coppolino prepared to perform a bedside percutaneous tracheostomy in a COVID+ patient.
How does one determine when to employ tracheotomy in COVID-19 patients requiring prolonged mechanical ventilation? It’s difficult to say given what relatively little we know about the disease at this point. Stephanie L. Nitzschke, MD, an acute care surgeon, trauma surgeon and surgical intensivist, is one of the clinicians developing guidelines on tracheotomy timing at Brigham and Women’s Hospital.
Dr. Nitzschke said that in order to balance the safety of patients and health care workers, the Brigham is delaying consideration of tracheotomy until 21 days after a positive test for COVID-19. But she stressed that all protocols related to this disease are subject to change. Read More
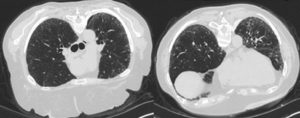
A soon-to-be published study reports a high prevalence of interstitial lung abnormalities (ILA) and undiagnosed interstitial lung disease (ILD) among first-degree relatives of patients with familial pulmonary fibrosis (FPF) and sporadic idiopathic pulmonary fibrosis (IPF). Results suggest screening might be warranted for undiagnosed relatives to facilitate early detection of PF.